| In-Network | Out-of-Network | In-Network | Out-of-Network | In-Network | Out-of-Network | |
| Annual Deductible |
||||||
| Individual | $3,000 | $6,000 | $6,350 | $19,050 | $2,000 | $4,500 |
| Family | $6,000 | $16,500 | $12,700 | $38,100 | $4,000 | $13,500 |
|
Coinsurance (what you pay) |
20% | 50% | 0% | 50% | 20% | 40% |
| Out-of-Pocket Max (includes deductible) | ||||||
| Individual | $5,500 | $16,500 | $6,350 | $19,050 | $6,000 | $13,500 |
| Family | $11,000 | $33,000 | $12,700 | $38,100 | $12,000 | $40,500 |
| Physician Services | ||||||
| Office Visit | 20% After deductible | 50% After deductible |
0% After deductible | 50% After deductible | $30 copay | 40% After deductible |
| Preventive Care | 100% Covered | 50% After deductible | 100% Covered | 50% After deductible | $0 copay | 40% After deductible |
| Hospital Services | ||||||
|
Inpatient/ Outpatient |
20% After deductible | 50% After deductible | 0% After deductible | 50% After deductible | 20% After deductible | Plan pays 60% |
| Emergency Room | 20% After deductible | 50% After deductible | 0% After deductible | 50% After deductible | $200 copay; then plan pays 100% | $200 copay; then plan pays 100% |
Welcome to Epiq
Benefits
Welcome!
Welcome to the Epiq Benefits e-Guide. We are excited to provide you with a wide variety of benefits options that enable you to select a comprehensive set of coverages that can help protect your health, your family, and your future.
At the center of your benefit options, you’ll find a set of competitive healthcare options through Cigna. At Epiq, our medical plans are self-insured. This means our company pays for all the claims. Because we are a self-insured group health plan, the overall cost and ultimately your paycheck contributions are impacted by your health care decisions. Choosing the ER when an Urgent Care facility is more appropriate or taking a brand name medication when a generic version is available not only costs you more money out of pocket, but costs Epiq and all enrolled employees more in the long run.
Being a smart consumer now will help keep costs more manageable in the future. Maintaining that behavior will benefit you and all enrolled employees by containing claims and therefore controlling the increase to your biweekly contributions. The information and resources included throughout this e-guide are designed to help us all make "healthy" choices.
Remember, we’re all in this together.
••••
Click Below to Get Started
Jump to the desired section using the buttons below







When & How to Enroll
Effective Dates
New Hires
Benefits are effective the first of the month following 30 days of continuous employment. Benefit elections must be made within a 21-day enrollment period from your date of hire through Workday.
If you do not elect benefits during the initial eligibility window, you will be required to wait until the next open enrollment period to enroll unless you experience a qualifying event.
Annual Enrollment
Benefits are effective on June 1, 2026. Benefit elections must be made within the annual enrollment process, April 15, 2026- April 29, 2026.
Qualifying Life Event
Benefits are effective based on the type of life event you are experiencing.
Examples: the birth of a child or marriage, coverage would be effective the day of the life event. Please see below for additional information.
Please click the appropriate Quick Start Guide to the right for detailed enrollment instructions.
Who is eligible for benefits?
You can enroll in our benefit programs if you are a full-time employee regularly working at least 30 hours a week. Temporary employees, part-time employees working fewer than 30 hours a week, and contractors are not eligible for benefits. Benefit deductions will be removed per paycheck on a 26 paycheck schedule annual basis.
In addition, you can enroll the following eligible dependents in most of our benefits plans:
- Spouse or domestic partner (see below for additional spouse/domestic partner eligibility information)
- Children up to age 26.
- Unmarried children of any age with a mental or physical disability that requires them to depend on you for support.
Upon completion of your enrollment task in Workday, you will be required to complete an e-signature to submit your elections. This will serve as your attestation that all dependents you have added to your plan meet the eligibility requirements.
Spouse/Domestic Partner Eligibility
If your spouse/domestic partner is eligible for healthcare coverage through their employer they will not be eligible for coverage through Epiq.
An eligible spouse/DP must meet one of the following:
-
Spouse/DP does not have access to health care through their employer
-
Spouse/DP is not employed
-
Spouse/DP is self-employed
-
Spouse/DP is employed in an Epiq benefits eligible position. If the employee and spouse both work for Epiq in a benefits eligible position they may choose to enroll in single, spouse or family coverage.
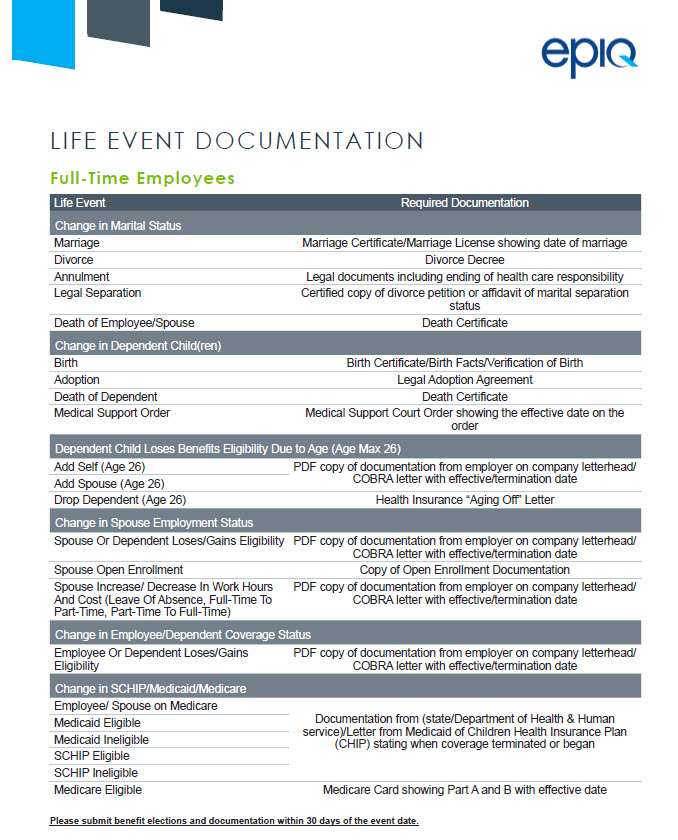
Qualifying Event Changes
The IRS limits the benefit changes you can make during the year for pre-tax benefit elections on medical, dental, vision, and FSA. Changes can be made outside the open enrollment period only if you and/or your family experiences a qualifying event. Please note, when experiencing a QLE to add a dependent, a plan change is not permitted, only adding that dependent to your current plan is allowed.
All changes must be requested through Workday within 30 calendar days of experiencing a qualifying life event.
Please note: You must complete the entire process in Workday within 30 days. Simply uploading documentation is not sufficient. Supporting documentation must be submitted, and changes must be made in your Workday benefit event within the 30 day period. If you have questions or need assistance with this process, please create a Workday Ticket
If you fail to submit the request and supporting documentation through Workday within 30 days, you will not be allowed to make benefit changes until the next open enrollment period.
If you are unaware of the documentation you need to submit, click the grid to the right.
CHOOSING A HEALTH PLAN JUST GOT EASIER
The Cigna Easy Choice tool helps you find the plan thats right for you and your family.
The Cigna Easy Choice tool gives you personalized guidance to help you find your best fit medical plan.
You can use it from just about anywhere. All you have to do is answer a few quick questions about your needs and preferences. Then, you’ll see available plans, ranked by what matters most to you. Compare your options side-by-side. Then print, save or email a handy checklist to use when you enroll.
Access code to get started:
QSHN-1653
Want more information?

Need help enrolling?
We are excited to provide our employees an enhanced, more personal way to understand the full range of all benefits offered at Epiq. Our Benefit Communication Specialists (BCS) are here to help you better understand our valuable core and voluntary benefits as well as assist you in the enrollment process. If you would like to speak with a BCS today, please call 844-600-7072 or create a ticket on Workday Help

Medical Benefits
Cigna Health Care
Epiq offers Cigna medical plans for you to choose from. All plans offer the convenience of referral-free access to doctors and the option (not requirement) to select a personal primary care physician. Keep in mind, you will have lower costs for services provided by in-network physicians.
Each plan's summary that highlights plan provisions may be found by clicking the buttons below.
2026 - 2027 Group Health Plan Details
Cigna Open Access Plus Network
| Plan Tier | Consumer-Driven Plan | Value Plan | Copay Plan |
| Employee Only | $83.48 | $46.36 | $162.38 |
| Employee + Spouse (DP) | $170.11 | $108.24 | $324.76 |
| Employee + Child(ren) | $164.58 | $104.77 | $313.81 |
| Employee + Family | $252.68 | $160.27 | $492.95 |
Cigna LocalPlus Network
| Consumer-Driven Plan | Value Plan | Copay Plan |
| $57.24 | $29.98 | $125.38 |
| $116.64 | $72.21 | $255.49 |
| $113.30 | $69.43 | $246.60 |
| $176.63 | $108.31 | $363.80 |
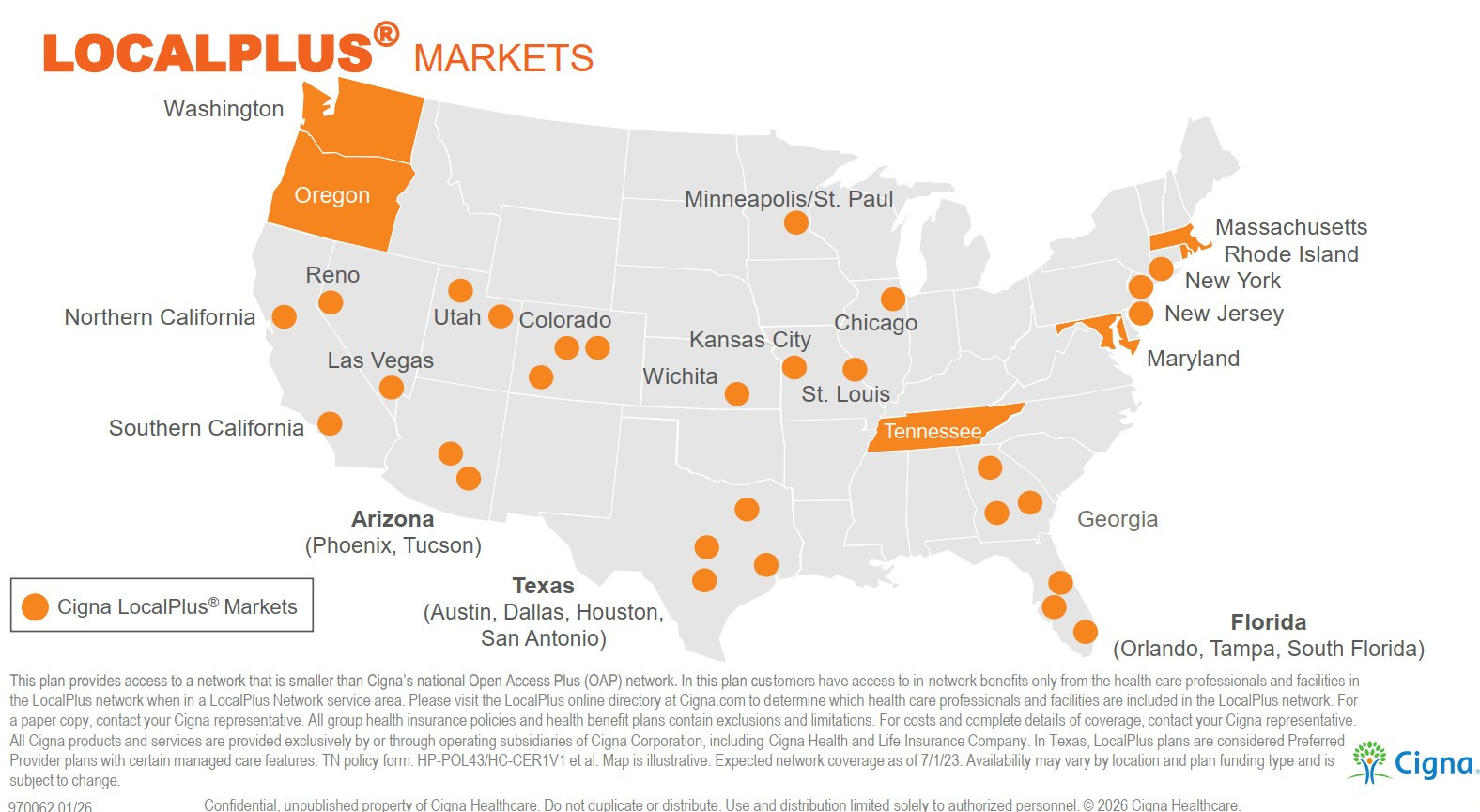
Cigna Local Plus Network
Employees who reside within the Cigna Local Plus Network will be placed in this network when enrolling in an Epiq medical plan.
Employees who reside outside these areas, will remain in the broader OAP Network.
Our three Local Plus medical plans provide access to high quality care and can save up to 35% on payroll deductions when moving from the broad network!
Participants living in the Local Plus markets who wish to opt-out of this network during Open Enrollment and enroll in the Open Access Plus network, with the corresponding payroll deductions must:
-
Contact EpiqBenefits@epiqglobal.com within 30 days of your Qualifying Event Date or within 21 days of your New Hire Date to request the change. Once you receive a confirmation email from the benefits team confirming that your Workday task has been reset, you will need to complete your new Workday enrollment task prior to Open Enrollment closing. If you have already emailed benefits in previous years, there is no need to email again, you will see both network options on your Workday benefit event.
-
NOTE: If you've already completed the enrollment you will be required to re-enter your elections.
-
Consumer Driven HSA & Value HSA Plans
These two high deductible health plans (HDHP) use in-network or out-of-network physicians with deductibles and coinsurances for services. Pharmacy benefits are subject to the deductible.
On both plans, all participants must meet the deductible before the coinsurance rate applies for medical services or pharmacy expenses.
On the Consumer Driven plan, there is one combined family deductible for the family tier coverage. Participants enrolled in the family tier coverage must satisfy the family deductible before the coinsurance will pay.
On the Value plan, if you have family members on the plan, each family member must meet their own individual deductible until the total amount of expenses meets the overall family deductible.
Traditional Copay Plan
This Plan uses in-network or out-of-network physicians with copays, deductibles, and coinsurances for services. Pharmacy benefits are not subject to the deductible. The pharmacy coinsurance rate is applicable from the first prescription filled.

Watch a helpful video on the difference between HDHP and Copay Plans
Healthy Pregnancy Healthy Babies
Cigna Healthy Pregnancies, Healthy Babies® is a comprehensive maternity condition management program for eligible Cigna members. This program aims to educate and support your Cigna patients at the very start of their pregnancies to ensure healthy pregnancies and babies by:
- Supplementing and enhancing the doctor-patient relationship
- Helping your patients better understand all aspects of their pregnancies so they can ask better questions and become better prepared to make decisions around testing, treatments for medical conditions and delivery
- Encouraging sensible prenatal behaviors, like quitting smoking, eating the right food and seeing a doctor regularly

Introducing Christopher Gonzalez, your dedicated Cigna Service Partner
Christopher Gonzalez is a customer service professional with over 15 years of experience, driven by a passion for helping others and creating positive experiences.
Christopher is recognized for his proactive communication style, problem-solving mindset, and genuine dedication to making a meaningful impact. His goal is to ensure every client feels supported, informed, and valued.
Christopher can help you:
- Understand your plan benefits.
- Find in-network healthcare providers and arrange care.
- investigate and answer questions regarding claims and authorizations.
- Resolve billing discrepancies.
- Provide education on Cigna Healthcare programs, services, and benefits available to you.
- Ensure you get the most from your health plan.

CHOOSING A HEALTH PLAN JUST GOT EASIER
The Cigna Easy Choice tool helps you find the plan thats right for you and your family.
The Cigna Easy Choice tool gives you personalized guidance to help you find your best fit medical plan.
You can use it from just about anywhere. All you have to do is answer a few quick questions about your needs and preferences. Then, you’ll see available plans, ranked by what matters most to you. Compare your options side-by-side. Then print, save or email a handy checklist to use when you enroll.
Access code to get started:
QSHN-1653
Want more information?

A Few Notes About Epiq Health Plans and Health Care Reform
All of the Cigna plans satisfy the minimum essential coverage requirement of the individual mandate. By enrolling in an Epiq plan, you are satisfying your requirement to have insurance coverage under the individual mandate. The plans are compliant with the provisions of the Affordable Care Act. Each plan year, the medical plans are reviewed to ensure they remain compliant with the ever-changing legislation.
These plans meet the Minimum Creditable Coverage provisions of the Massachusetts Health Insurance Requirements.

Prescription Benefits
Rightway Rx
Epiq’s pharmacy benefits are through Rightway. The pharmacy costs are built into your medical plan costs and deductibles, coinsurance and out-of-pocket maximums are all tied to the medical plan you enroll in.
|
|
Consumer-Driven |
HSA Value Plan |
Traditional |
| 30-day Supply Retail Pharmacy |
|||
| Generic |
20%
after deductible
|
0% after deductible
|
20%
($15 min; $50 max)
|
| Preferred |
20%
after deductible
|
0% after deductible
|
20%
($35 min; $100 max)
|
|
Non-Preferred |
35%
after deductible
|
0% after deductible
|
20%
($75 min; $200 max)
|
|
Specialty |
20%
after deductible
|
0% after deductible
|
20%
($50min; $200 max)
|
| 90-day Supply Retail and Mail Order Pharmacy | |||
| Generic |
20%
after deductible
|
0% after deductible
|
20%
($15 min; $100 max)
|
| Preferred |
20%
after deductible
|
0% after deductible
|
20%
($75 min; $200 max)
|
| Non-Preferred |
35%
after deductible
|
0 % after deductible
|
20%
($125 min; $400 max)
|
| Specialty | Not Covered | Not Covered | Not Covered |


This is text content
Health Savings
Account
What is a Health Savings Account?
A health savings account (HSA) is a savings account used in conjunction with a high deductible health plan. It allows users to save money on a pre-tax basis to use for qualified health expenses. Simply decide how much to contribute during enrollment, and funds are deducted from your paycheck on a pre-tax basis.**
The Health Savings Account is managed by Cigna’s banking partner, HSA Bank. If you enroll in the Consumer-Driven or Value HSA plans, an account will be opened with HSA Bank on your behalf and you’ll receive a debit card in the mail.
What are the advantages?
You're in charge - Employees can decide how much they want to contribute to their HSA, to spend or save the funds in the account, and even invest the funds similar to a 401(k) retirement account.
You own it & you keep it - Remember, you own this account, which means the account and the funds go with you beyond your employment with Epiq. When you turn age 65, the account can then be used toward retirement expenses such as medicare premiums and long-term care.
Triple Tax Savings - Deposits into the account, payments or reimbursements for eligible expenses, and interest or earnings on investments are all TAX FREE.
Don't leave money on the table!
Epiq will contribute to your HSA! Once the plan starts, Epiq will match $1 for $1 each pay period up to the below limits:
-
Employee Only - $750 per year
-
Employee + 1 (or more) - $1,250 per year
** You will make your election based on the Epiq plan year June 1-May 31. Please note that the IRS limits the HSA contributions on a calendar year basis. It is each employee’s responsibility to ensure they do not over-contribute to the HSA. Consult your tax advisor as appropriate.

Watch a short video to get familiar with an HSA.
2026 IRS Contribution Limits
How Before-Tax Dollars Save You Money
Using the following example, an Epiq employee and spouse have a combined household income of $40,000 a year. They estimate that they will spend $2,000 in out-of-pocket healthcare expenses this year. Their total contribution to the health savings account is $3,000. Here is how they save on taxes. (The below example assumes the couple files a married/joint tax return).
|
|
With Before-Tax Dollars | With After-Tax Dollars |
| Annual Gross Salary | $40,000 | $40,000 |
| HSA Contributions | ($3,000) | $0 |
| Taxable Income | $37,000 | $40,000 |
| Estimated Federal Income Tax | ($4,684) | ($5,134) |
| Social Security (FICA) Tax | ($2,830) | ($3,060) |
| Income After Taxes | $29,486 | $31,806 |
| After-Tax Payments for Health Care | $0 | ($3,000) |
| Spendable Income | $29,486 | $28,806 |
This example is only an estimate of possible savings. It does not include any state or local tax savings. Your actual savings will vary based on your annual income, your income tax filing status, and your contributions to the health savings account. Please note that some states still impose state income tax on health savings account contributions. Check with your tax advisor.

Wellness Incentive
Program
Join Epiq's Wellness Incentive Program, WellRight!
Who is eligible?
What's in it for me?
Point Structure

FAQs
What do I need to do to earn points?
Once you earn 25,000 points, you will earn a medical premium discount of $23.07 per paycheck ($600 annually) for the rest of the plan year (ending May 31,2027). If you earn 50,000 points prior to May 31, 2027, you will also earn the credit for the 2027-2028 plan year (ending May 31, 2028).
How can I confirm if I am receiving the discount?
Within 2 pay periods, your wellness credit will automatically appear on your paycheck once you earn the points.
Is participation mandatory?
Participation in this program is completely voluntary. However, enrolling is the only way to earn the premium credit. Beyond that, the program is designed to support your personal wellness goals—helping you track progress, stay motivated, and build healthy habits over time.


Dental & Vision Benefits
Cigna Dental
Epiq offers two Cigna dental plans from which to choose: Dental PPO and Dental DHMO.
Dental PPO
This plan offers the convenience of visiting any dentist you wish without designating a primary care dentist or obtaining a referral for a specialist visit. Coverage levels are not reduced if you choose to visit a non-network dentist; however, because the dentists in the DPPO Core Network have agreed to provide services at guaranteed rates, you may save money when using an in-network dentist. Dentists outside of the Cigna network may bill you for the difference between Cigna’s allowed charge and the dentist’s rate for service.
Dental DHMO
This plan includes coverage for many procedures that may not be available on other dental plans. There are no deductibles to pay before coverage begins, no annual dollar maximums on covered services, no claim forms, and no waiting periods.

Cigna Dental Cards
Cigna does NOT issue dental identification cards. Your provider should be able to verify your coverage directly with Cigna. If they are unable to do so, you can print a dental card after registering at www.myCigna.com.
|
|
DPPO |
DHMO |
| Deductible |
||
| Individual | $50 | Refer To Summary of Benefits |
| Family | $150 | Refer To Summary of Benefits |
| Preventive covered without deductible? | Yes | Refer To Summary of Benefits |
| Coinsurance (portion you pay) | ||
| Preventive Services I (subject to deductible for Low Plan) | 0% (covered 100%) | Refer To Summary of Benefits |
| Basic Services II (subject to deductible) | 20% | Refer To Summary of Benefits |
| Major Services III (subject to deductible) | 50% | Refer To Summary of Benefits |
| Orthodontic (no deductible & dependent child(ren) to age 19 only) | 50% | Refer To Summary of Benefits |
| Benefit Maximum | ||
| Calendar Year Maximum | $1,500 | Refer To Summary of Benefits |
| Lifetime Orthodontia Maximum | $1,500 | Refer To Summary of Benefits |
What you will pay bi-weekly for each plan:
| DPPO | DHMO | |
| Employee Only | $12.04 | $6.93 |
| Employee + Spouse or Domestic Partner | $21.80 | $13.39 |
| Employee + Child(ren) | $30.47 | $18.53 |
| Employee + Family | $41.36 | $23.85 |
EyeMed Vision
Epiq’s vision benefit through EyeMed Insight Vision Care Network offers discounts for exams, lenses, and contacts at in-network and out-of-network coverage levels. The plan also provides a 15% savings off the retail price for LASIK and PRK procedures performed at all US Laser network centers.
EyeMed has a network of over 30,000 providers that include private optometrists, opticians and the nation’s leading retailers, including Target Optical, LensCrafters and Pearle Vision locations.
Out-of-network benefits offer more flexibility; however, there are lower coverage levels for using an out-of-network provider.
Keep in Mind! If a provider is in the PLUS Network, there is a $0 copay on eye exams + an extra $50 frame allowance can be applied.

What you will pay bi-weekly:
| Employee Only | $3.02 |
| Employee + Spouse or Domestic Partner | $5.72 |
| Employee + Child(ren) | $5.76 |
| Employee + Family | $9.12 |

WEX Flexible Spending
Accounts & Commuter
Flexible Spending Accounts
Epiq offers four Flexible Spending Account (FSA) options with Wex. An FSA is a program that permits benefits-eligible employees to pay for eligible expenses with pre-tax dollars through payroll deduction.
The money deposited into these accounts is not taxed at the time of contribution and remains tax-free when it is withdrawn as reimbursement or payment for eligible expenses. The qualified expenses and contribution limits for each plan are regulated by the IRS.
Healthcare FSA
Funds in the healthcare FSA can be used to pay for eligible medical, dental, and vision expenses, including deductibles and copayments that are not covered under any other plan. You will also receive a debit card linked to your account, which can be used to pay for services rather than submitting a claim for reimbursement. Remember, if you elect the Epiq HSA plans, you are not eligible to contribute to the healthcare FSA.
-
The maximum annual healthcare contribution for 2026 is $3,400
Dependent Care FSA
Funds in the dependent care FSA can be used to pay for dependent or elder care expenses that enable you to work. The IRS states that dependent care flexible spending account (FSA) elections are irrevocable and cannot be changed during the period of coverage unless there is a permitted change in election based on a qualified life event.
-
The maximum annual dependent care contribution for 2026 is $5,000 per household or $2,500 if married, filing separately.
HealthEquity/WageWorks
Effective June 1, 2026, Wex replaced HealthEquity/WageWorks. If you have past claims that still need to be submitted to HealthEquity, please contact them at 866.346.5800.


Watch a short video on how to optimize your FSA.
More helpful information:
WEX Commuter Transit and Parking
You can make monthly elections for transit and parking on Workday. Elections will be effective within two pay periods.
To elect or make changes go to the Change Benefits task in Workday, followed by Commuter Election Change.
- The 2026 maximum monthly pre-tax transit contribution is $340
Commuter contributions are regulated by the IRS on a monthly basis; therefore, your payroll deductions will be withheld only from the first and second paychecks of each month. In months where there are three paydays, the third check will not have a deduction for pre-tax transit and/or parking elections.

Watch a short video on commuter benefits.
Eligible Mass Transit Expenses
- Buses
- Trains and subways
- Ferries
- Vanpools
Eligible Parking Expenses
- Parking at or near your place of employment
- Parking at a location from which you commute to work
Ineligible Transportation Expenses
- Gas
- Mileage
- Bridge or highway tolls
- Expenses for someone other than you
- Carpool or taxi (unless the vehicle meets the requirements for vanpooling)
More helpful information:
How Before-Tax Dollars Save You Money
Using the following example, an Epiq employee and spouse have a combined household income of $40,000 a year. They estimate that they will spend about $1,000 in eligible day care expenses for their child and $2,000 in out-of-pocket healthcare expenses this year. Their total contribution to the flexible spending account is $3,000. Here’s how they save on taxes. (The below example assumes the couple files a married/joint tax return.)
|
|
With Before-Tax Dollars | With After-Tax Dollars |
| Annual Gross Salary | $40,000 | $40,000 |
| FSA Contributions | ($3,000) | $0 |
| Taxable Income | $37,000 | $40,000 |
| Estimated Federal Income Tax | ($4,684) | ($5,134) |
| Social Security (FICA) Tax | ($2,830) | ($3,060) |
| Income After Taxes | $29,486 | $31,806 |
| After-Tax Payments for Health Care | $0 | ($3,000) |
| Spendable Income | $29,486 | $28,806 |
This example is only an estimate of possible savings. It does not include any state or local tax savings. Your actual savings will vary based on your annual income, your income tax filing status, and your contributions to the spending accounts. Please note that some states still impose state income tax on spending account contributions. Check with your tax advisor.
Use It or Lose It Rule — Plan Regulation
IRS regulations require that expenses must be incurred in the current plan year in order to receive reimbursement. Therefore, it is important to budget carefully when you set up your FSA so that you do not contribute more than you will spend. If your employment should terminate, eligible expenses must be incurred prior to the end of your employment. Healthcare FSA participants will be allowed to carry over up to $680 of unreimbursed FSA funds to the following plan year. If your employment should terminate, either voluntary or involuntary, eligible expenses must be incurred prior to your last day of employment. Any funds unused in your FSA account will be forfeited and, per IRS regulation, cannot be reimbursed back to you.
All healthcare and dependent care FSA claims must be submitted by August 31 2026, for the 2025/2026 plan year for eligible services rendered on or before May 31, 2026. Please contact HealthEquity/WageWorks at 866.346.5800

Life & Disability
New York Life Disability Insurance
Epiq provides an employer-paid basic short-term disability (STD) plan and an employee-paid long-term disability (LTD) insurance to eligible employees at group insurance rates. Employees will be automatically enrolled in the basic STD plan but must elect coverage for the LTD plans.
For information regarding state- funded disability programs please contact epiqbenefits@epiqglobal.com

Watch a short video about disability insurance.
Short-Term Disability
Company provided short-term disability benefits are designed to replace a portion of your income for a non-work-related short-term injury or illness.
What am I eligible for?
On the first of the month following 30 days of service, participants are eligible to receive 60% of weekly covered earnings to a maximum of $1,500 per week, beginning 14 calendar days following the accident or illness, for up to 11 weeks.
Supplemental Maternity Leave
Epiq's maternity leave policy provides paid leave for employees who give birth to recover from childbirth and to care for their newborn.
All full-time US employees working 30 or more hours per week that have been employed for 12 consecutive months and are on an approved disability claim for maternity leave through New York Life, are eligible to receive this benefit. In some cases, you may be auto approved for coverage. If not, New York Life will review your application and contact you if more information is required. In all cases, they will notify you of your application outcome.
Employees are eligible for up to 10 weeks of maternity leave, which must be taken as one continuous period and may not be split, deferred, or taken intermittently. Through a combination of short-term disability benefits and employer-provided supplemental pay, eligible employees will receive 100% of their regular weekly earnings during the period in which short-term disability benefits apply. New York Life will administer the maternity leave payments, coordinating the supplemental pay to ensure total weekly earnings equal 100% while short-term disability benefits are in effect. Any remaining approved maternity leave beyond the paid period will be unpaid unless otherwise required by applicable law or policy.

Watch a short video about short-term disability.
Long-Term Disability
If you are still disabled after your short-term disability benefits have ended and you have elected long-term disability, your claim will automatically transition to the long-term disability program. Long-term disability insurance supplements your income in the event you are unable to work due to a covered disability that lasts longer than 90 days. New York Life must review and approve your LTD claim before benefits are payable.
The long-term disability benefit pays 60% of your covered monthly earnings, up to a monthly maximum of $10,000. Because you pay the premiums for your disability insurance with after-tax dollars, amounts paid out under the long-term disability plan are not subject to taxes. Benefits are payable until the earliest of: (1) the date on which the covered participant is no longer totally disabled, (2) the end of the maximum benefit period, (3) the participant reaches Social Security Normal Retirement Age (SSNRA), or (4) the date of the participant’s death.
Long-term disability benefits are reduced if you are receiving income from other sources during your disability. The plan may limit benefits or disabilities caused or contributed to by mental/nervous conditions or drug/alcohol abuse. Benefits are not payable under certain circumstances such as commission of a felony, attempted suicide, self-inflicted injury, or war.
How to File a Claim
To request a leave of absence and report a claim, you will contact New York Life at 888-842-4462 or CLICK HERE

Watch a short video about long-term disability.
- Be the parent of a child who was born or adopted or be the foster parent of a foster child who has been placed (the child must be age 17 or younger).
- Please note: If taking maternity leave as well, the paid parental leave would bring the overall total to 12 weeks paid at 100%.
- Employees must take paid parental leave in one continuous period of leave and must use all paid parental leave during the 12 month time frame indicated above. Any unused paid parental leave will be forfeited at the end of the 12 month time frame.
New York Life: Life Insurance
Epiq provides a variety of term life insurance plan options. These plans provide individuals and their families with financial protection and peace of mind.
Basic Life and AD&D Insurance
Epiq provides an employer-paid Basic Employee Life and Accidental Death & Dismemberment (AD&D) insurance equal to 1x your salary, up to a maximum of $250,000.
Basic Life & AD&D coverage over $50,000 will have imputed income on the paycheck.
NOTE: Employee supplemental life insurance coverage must be elected in order to be eligible to purchase spouse/domestic partner and/or child(ren) life coverage.
Supplemental Life Insurance
In addition to the employer-paid coverage, you have the opportunity to elect supplemental life insurance for yourself, your spouse/domestic partner, and children.
Employee Coverage
Minimum: $10,000
Maximum: Lesser of 5x annual compensation OR $500,000
Increments of: $10,000
Guaranteed Issue* : $250,000
Spouse/Domestic Partner Coverage
Minimum: $5,000
Maximum: $500,000
Increments of: $5,000
Guaranteed Issue* : $50,000
Child(ren) Coverage
Benefit Amount: $10,000 ($1,000 < six months)
Guaranteed Issue* : $10,000
*Guaranteed Issue amounts are only available upon initial offer of coverage as a new hire or newly eligible employee.
What happens next?
In some cases, you may be auto-approved for coverage. If not, the carrier will review your application and contact you if more information is required. In all cases, NYL will notify you of your application outcome.
Voya: Premier Whole Life Insurance
Whole life insurance is a portable form of life insurance that is designed to provide long-term insurance protection for you during your working years and beyond. The coverage amount that is chosen and the policy premiums are guaranteed to be fixed for the life of the policy as long as the required premium payments are met.
Also available as a rider to your life insurance policy, long-term care coverage provides monthly payments in the event that you require assistance with activities of daily living. Qualifying care includes home healthcare, adult day care, or confinement to a long-term care facility.
For these programs rates are determined upon several factors. For questions on rates and plan designs, please contact your Benefit Communication Specialists.
For Whole Life Questions, please contact 844-600-7072

401(k) Retirement

It's never too late to get started!
At Epiq, we are committed to supporting our employees’ total wellbeing by offering meaningful and competitive benefit options. When it comes to your financial wellness, Epiq offers a 401(k) plan with Fidelity that can help you stay on the path towards reaching your retirement goals.
Eligibility
All Epiq employees are eligible to participate in the 401(k) retirement plan following the completion of one month of service. Once becoming eligible, participants must enroll directly with Fidelity at www.401k.com or by calling 800-835-5097
401(k) Employer Match
On a bi-weekly basis, Epiq will match 2.5% of an employees contribution for ALL participants who are actively contributing to their 401(k). The Epiq match will be 100% vested after three years of vesting service.
Don't leave money on the table!
Epiq's discretionary match represents an investment by Epiq to help you reach your retirement goals. Don't miss out by leaving this money that Epiq has already allocated on the table.
To take full advantage of the company match, update your contributions with Fidelity today by logging in to www.401k.com or calling the Fidelity Customer Service Center at 800-835-5097.
More helpful information:
Get the financial help you’re looking for—all in one place
No matter what is happening in your life right now, one thing is certain—Fidelity can help. Fidelity can help answer your questions and explore opportunities on topics ranging from getting back on track with your retirement savings to dealing with market changes to managing day-to-day budgeting concerns.
Visit NetBenefits.com/GetHelp and explore a broad range of current topics, all in one place.

Voluntary Benefits
Critical illness
Critical illness insurance provides lump sum payments for specific serious illnesses such as heart attack, stroke, coronary artery bypass, major organ transplant, kidney failure and cancer. Payments are made directly to you, not to the doctors, hospitals or other health care providers. The payment is yours to spend as you see fit and may be used to cover high deductibles or even ongoing household expenses such as mortgage or car payments.
Click below to learn more!
Accident Insurance
Accident insurance is designed to provide you cash payments if you experience covered injuries such as dislocations, fractures, loss of limbs, death, or disability. It can help you with out-of-pocket costs that your medical plan doesn’t cover, like deductibles and coinsurance. It covers accidents that occur off the job. Also included are benefits for accident-related expenses such as hospital admission and ER care.
Your Bi-Weekly Contributions
Employee Only = $4.56
Employee + Spouse/DP = $7.39
Employee + Child(ren) = $8.75
Employee + Family = $11.58
NY & RI GBTS Weekly Contributions
Employee Only = $2.28
Employee + Spouse/DP = $3.70
Employee + Child(ren) = $4.38
Employee + Family = $5.79
Hospital Indemnity Insurance
Hospital indemnity insurance helps covered employees and their families cope with the financial impacts of a hospitalization. You can receive benefits when you’re admitted to the hospital for a covered accident, illness, or childbirth. The money is paid directly to you — not to a hospital or care provider. The money can also help you pay the out-of-pocket expenses your medical plan may not cover, such as coinsurance and deductibles.
Your Bi-Weekly Contributions
Employee Only = $10.59
Employee + Spouse/DP = $22.32
Employee + Child(ren) = $16.75
Employee + Family = $28.48
NY & RI GBTS Weekly Contributions
Employee Only = $5.30
Employee + Spouse/DP = $11.16
Employee + Child(ren) = $8.38
Employee + Family = $14.24
Pet Insurance
Pet insurance is an insurance policy pet owners buy to help cover their pet’s health care expenses. Policyholders pay a monthly fee and can be reimbursed for certain medical expenses. Some of the things a policy with MetLife Pet can typically cover are:
- Accidents and illnesses
- Vet-prescribed medication
- Surgeries, hospitalization, and emergency care
- Diagnostic testing, including blood tests, X-rays, and more
- Alternative therapies
MetLife Pet also offers an optional preventive care plan that can help cover costs related to things like vaccinations, parasite treatment and prevention, teeth cleaning, and more.
Essentially, pet insurance can help you give your furry family members the care they need without worrying as much about unexpected expenses.
Click on the links below to see cost information and to enroll
Legal Insurance
Reduce the out-of-pocket cost of legal services with MetLife Legal Plans. With network attorneys available in person, by phone or by email and online tools to do-it-yourself — MetLife makes it easy to get legal help. And, you will always have a choice in which attorney to use
Your Bi-Weekly Contributions
Employee = $9.69
NY & RI GBTS Weekly Contributions
Employee = $4.85

Digital Wellness Benefit
Make the internet a safe place for you and your loved ones with DigitalGuard Complete plan through Aura
Aura protects your personal info, finances, and devices from fraud. They will detect and resolve online threats before they happen.

Do you shop online, connect to WiFi, or own a smartphone or tablet? If so, you need Aura to protect the things that matter to you the most: your identity, money & assets, family & reputation, and privacy. Aura provides you and your loved ones with a digital security benefit that’s simple, so it’s easy to stay safe online.
Meet Aura, the new standard in digital security.
Aura will let you know if your online accounts and passwords are at risk, and work with you to keep them safe. If changes to your credit or bank accounts are detected - or if there is suspicious spending activity on your accounts - you'll receive real-time alerts and have a dedicated Case Manager to work with you to resolve it. Aura also gives you the confidence to stream, shop, and bank online privately and securely with military-grade encryption and powerful antivirus protection. Plus, every member is backed by $1M insurance* to cover eligible losses and fees due to identity theft and fraud.
Identity
The fastest alerts with direct 3 bureau integation and AI-driven technology.
Network/WiFi Security
Fast connection speeds and broad coverage
Privacy
Aura provides automated, proactive list removal and masked data for additional protection
How To Use The Plan
After enrolling on Workday, you can access your account at www.my.aura.com/start to get started!

Lifestyle Benefits

Create a request in Workday: Complete the Adoption Assistance Request Form and/or Surrogacy Assistance Request Form and provide supporting documentation (receipts, invoices, legal documents) to the Benefits department.
-
-
Enter Create Request in the search bar on Workday
-
Search either: Adoption Assistance Request Form or Surrogacy Assistance Request Form
-
complete and submit
-
Approval Process: The Benefits department will review your application and notify you of approval within 30 days.
Receive Reimbursement: Approved reimbursements will be processed through payroll and included in your next paycheck.
Surrogacy & Adoption
We are proud to announce the launch of Epiq’s new Family Forming Benefits program on July 16th 2025—an initiative designed to support employees on their journey to parenthood through adoption or surrogacy. This benefit reflects our commitment to inclusive, compassionate support for all employees and their families.


Cancer is most treatable and least costly when caught early. Color identifies risk, gets people screened, and moves quickly on 100% of abnormal results to maximize care.
Sign up today at color.com/epiq
*all medically enrolled employees are eligible


Medicare Support
We have partnered with SmartConnect to provide all employees year-round access to free Medicare resources, personalized guidance, and enrollment services. SmartConnect makes the transition to Medicare easier than ever by offering free Medicare resources and one-on-one consultations with licensed insurance agents. This service is beneficial to anyone 64 ½ or older (or otherwise eligible for Medicare), including your family members and friends
How does it work?
- Learn about Medicare from a trusted industry professional.
- Understand what affects your health care costs and coverage options.
- Compare your current health coverage (whether it’s employer coverage or another plan) to multiple Medicare options.
- If you find a Medicare plan that meets your needs, SmartConnect helps you enroll immediately.


PerkSpot is a FREE, one-stop-shop for exclusive discounts to hundreds of your favorite national and local merchants. Use PerkSpot to find deals on everything from household essentials to once-in-a-lifetime vacations!
How to gain access:
All employees will have an email from PerkSpot in their Epiq inbox that will include a personal link to get set up.
Troubleshooting:
-
Double check your Junk Inbox
- If you need the email resent, please reach out to:
- 1-866-606-6057 or
- cs@perkspot.com
What kinds of discounts can I get from PerkSpot?
- Restaurants
- Tickets & Entertainment
- Computers & Electronics
- Travel & Hotels
- Apparel
- Home, Garden & Pets
- Cell Phones
- Flowers & Gifts

Active & Fit Direct
The Active & Fit Direct program offers fitness center memberships for $28 a month with access to thousands of gyms and studios, including standard gyms and premium options with discounts, and also includes on-demand workout videos. All employees are eligible regardless of medical plan enrollment status.
Get started today by signing up HERE! The Active&Fit link will be listed under Additional Benefits on the Epiq Benefits Workday portal.


Employee Support
Program
Employee Support Program
At some point in our lives, each of us face difficult situations. When these instances arise, Epiq’s new SupportLinc employee support program will be there to help.
This program is a confidential resource designed to help you deal with life’s challenges and the demands that come with balancing home and work; it provides you access to professional counseling as well as expert referrals to address a wide array of concerns.
SupportLinc upholds strict confidentiality standards. No one, including Epiq, will know who accesses the program unless participants specifically grant permission or express a concern that presents a legal obligation to release information.
Anger Management | Work Related Pressures | Stress
Expert Referrals and Consultation

Assistance the way you choose
More helpful information:

Carrier Contacts
Medical Plan - Cigna
Account #: 2471098
Phone: 800-244-6224
Website: www.mycigna.com
Claims Mailing Address:
Medical Claims, P.O. Box 182223, Chattanooga, TN 37422
Life and AD&D/Disability and Leave of Absence -New York Life
Life Insurance: FLX970843
STD: LK753222
FMLA: FML753222
LTD: VDT963791
Phone: 888-842-4462
Website: NYL Homepage
Dental Plan - Cigna
Account #: 2471098
Phone: 800-244-6224
Website: www.mycigna.com
Claims Mailing Address:
Dental Claims, P.O. Box 1-8037, Chattanooga, TN 37422
Rightway Rx - Pharmacy
Phone: 833-742-0298
Email: rwrx@rightwayhealthcare.com
Website: www.member.rightwayhealthcare.com
Vision Plan - EyeMed
Account #: 9811639
Phone: 866-800-5457
Website: www.eyemedvisioncare.com
Claims Mailing Address:
EyeMed Vision Care, Attn: OON Claims, P.O. Box 8504, Mason, OH 45040
Critical Illness, Accident, Hospital Indemnity- New York Life
Critical Illness: GCI100228
Accident: GAI100228
Hospital Indemnity: GHI100228
Phone: 888-842-4462
Website: NYL Homepage
SmartConnect: Medicare Assistance
Flexible Spending Accounts
Commuter/Transit - WEX
Phone: 866-451-3399
Claims Website: www.benefitslogin.wexhealth.com
Claims Mailing Address:
P.O. Box 2926 Fargo ND 58108
Health Savings Account - HSA Bank
Account #: 2471098
Phone: 800-244-6224
Website: www.mycigna.com
Claims Mailing Address:
HSA Bank, P.O. Box 939, Sheboygan, WI 53082-0939
COBRA Administration - Taben
Account #: 5921
Phone: 800-675-7341
Website: www.taben.com
Claims Mailing Address:
Taben Group (COBRA), P.O. BOX 7330, Shawnee Mission, KS 66207
Employee Support Program - SupportLinc
Phone: 888-881-LINC (5462)
Text SUPPORT to 51230
Website: www.supportlinc.com
Pet Insurance - MetLife
Account #:
Phone: 866-937-7387
Website: MetOnline - Common Access (metlife.com)
Legal Insurance - MetLife
Account #: 990-7977
Phone: 800-821-6400
Website: www.members.legalplans.com
Active & Fit Direct
Phone: 1-844-646-2746
PerkSpot
Phone: 1-866-606-6057
Email: cs@perkspot.com